❓ Why Do People with Heart Disease Need a Pacemaker?
And is it possible not to have one?
A pacemaker is a medical device used for certain heart conditions—especially abnormally slow heart rates or problems with the heart’s electrical conduction. It delivers small electrical impulses to help the heart beat at an appropriate rate so blood can circulate adequately, reducing the risk of fainting, heart failure, or sudden death.
🔎 Why is a pacemaker needed?
-
Bradycardia (slow heart rate)
-
Heart rate below 60 beats per minute can reduce blood flow to the brain and organs.
-
Symptoms may include dizziness, lightheadedness, fatigue, or fainting.
-
A pacemaker helps restore a steady, sufficient heart rate.
-
-
Arrhythmias (irregular heart rhythms)
-
For example, irregular rhythms, sometimes alongside coronary artery disease.
-
A pacemaker can regulate rhythm and prevent danger from severe arrhythmias.
-
-
Conduction disorders (Heart block)
-
Abnormal electrical signal conduction from the atria to the ventricles.
-
This can cause slow or irregular heartbeats.
-
A pacemaker substitutes for the heart’s faulty electrical system.
-
-
Preventing heart failure
-
Frequent rhythm problems can overwork the heart and lead to failure.
-
A pacemaker lowers this risk and helps preserve heart function.
-
⚠️ Can you choose not to get a pacemaker?
-
If a doctor determines it’s “necessary,” refusing the device may carry high risks such as frequent fainting, cardiac arrest, or sudden death.
-
In milder cases, monitoring may be advised first, but worsening symptoms often mean a pacemaker will still be needed.
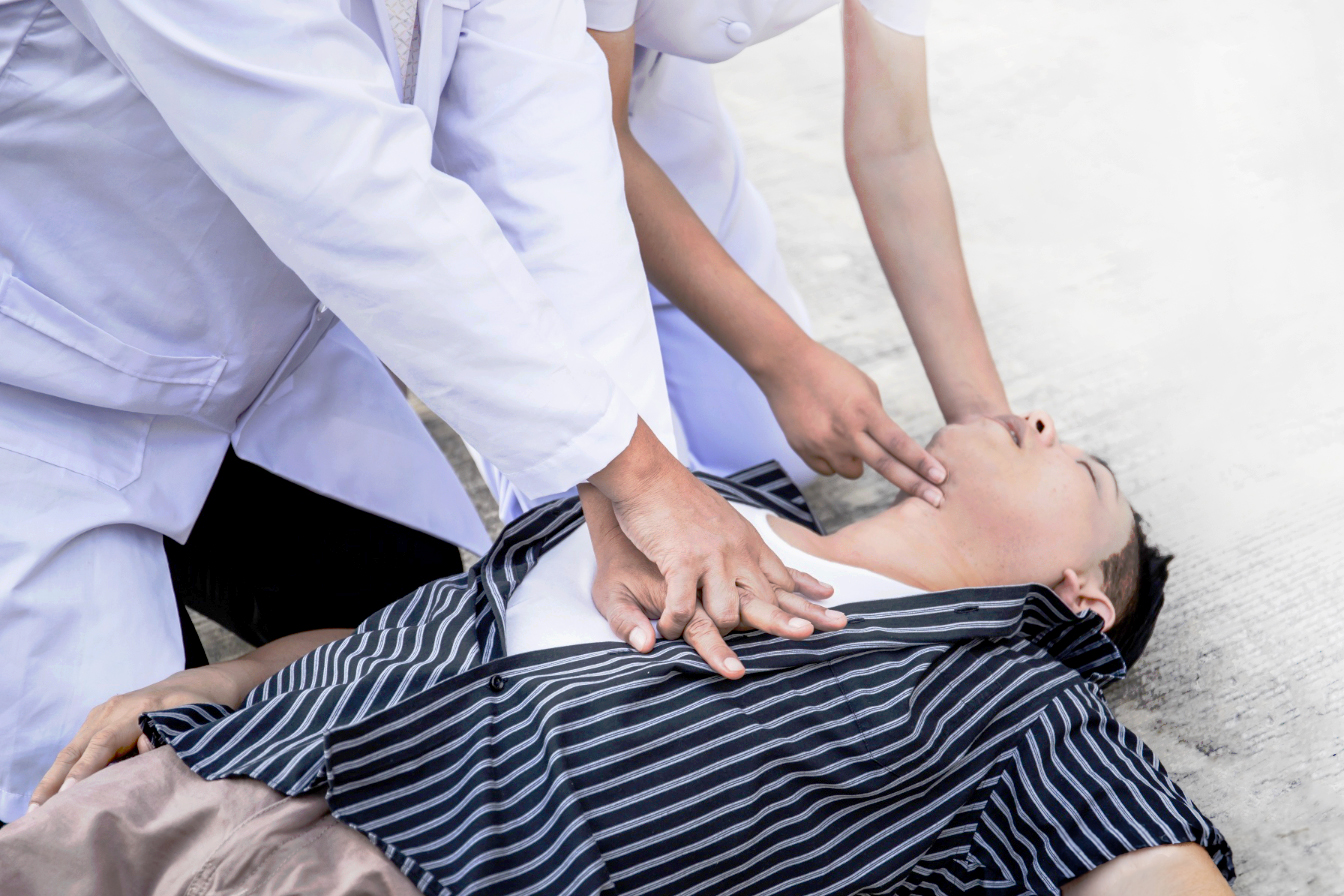
❓ What happens if you don’t get a pacemaker?
For patients who medically need a pacemaker but do not receive one, serious health and life-threatening consequences may occur:
1. Fainting (syncope)
Insufficient blood flow to the brain leads to low oxygen, causing dizziness, blackouts, or frequent fainting.
2. Heart attack/heart failure
Inadequate oxygen to the myocardium can damage heart cells and cause heart failure—life-threatening without timely treatment.
3. Reduced quality of life
Daily activities become difficult—physically and emotionally—making walking, exercising, or working much harder.
👩⚕️ Living with a Pacemaker
Most pacemaker patients can live near-normal lives, but a few lifestyle adjustments help protect health and the device.
Lifestyle adjustments
-
Follow medical instructions strictly.
-
Avoid strong magnets or devices that may interfere.
-
Do light exercise—walking, stretching, low-impact activities.
-
Avoid smoking and excess caffeine; choose heart-healthy foods.
-
Get adequate sleep.
🩹 Post-op wound care
-
Keep the wound dry for the first 5–7 days.
-
Do not scratch, press, or rub the incision.
-
Avoid heavy lifting or excessive use of the arm on the device side for 4–6 weeks.
-
Wear loose clothing that doesn’t irritate the wound.
-
Clean and change dressings as instructed.
🏃♂️ Activities you can do
-
Leisure or brisk walking.
-
Light exercise such as yoga or stretching.
-
Return to routine daily tasks (with doctor’s approval).
-
Drive or travel—consult your doctor first.
🩺 Follow-up care
-
Device checks every 2–6 months.
-
Assess the incision and overall symptoms.
-
Monitor battery life and adjust settings if needed.
🌟 Enjoying life after implantation
-
Stay positive and accept changes.
-
Care for both body and mind.
-
Maintain supportive relationships.
-
Set goals and keep favorite activities.
🔋 How long does a pacemaker last?
-
Battery life averages 7–10 years (depending on usage and settings).
-
When the battery depletes, a minor surgery replaces it, while the main device can last for decades if functioning normally.
-
Full system replacement isn’t needed unless there’s a device issue.
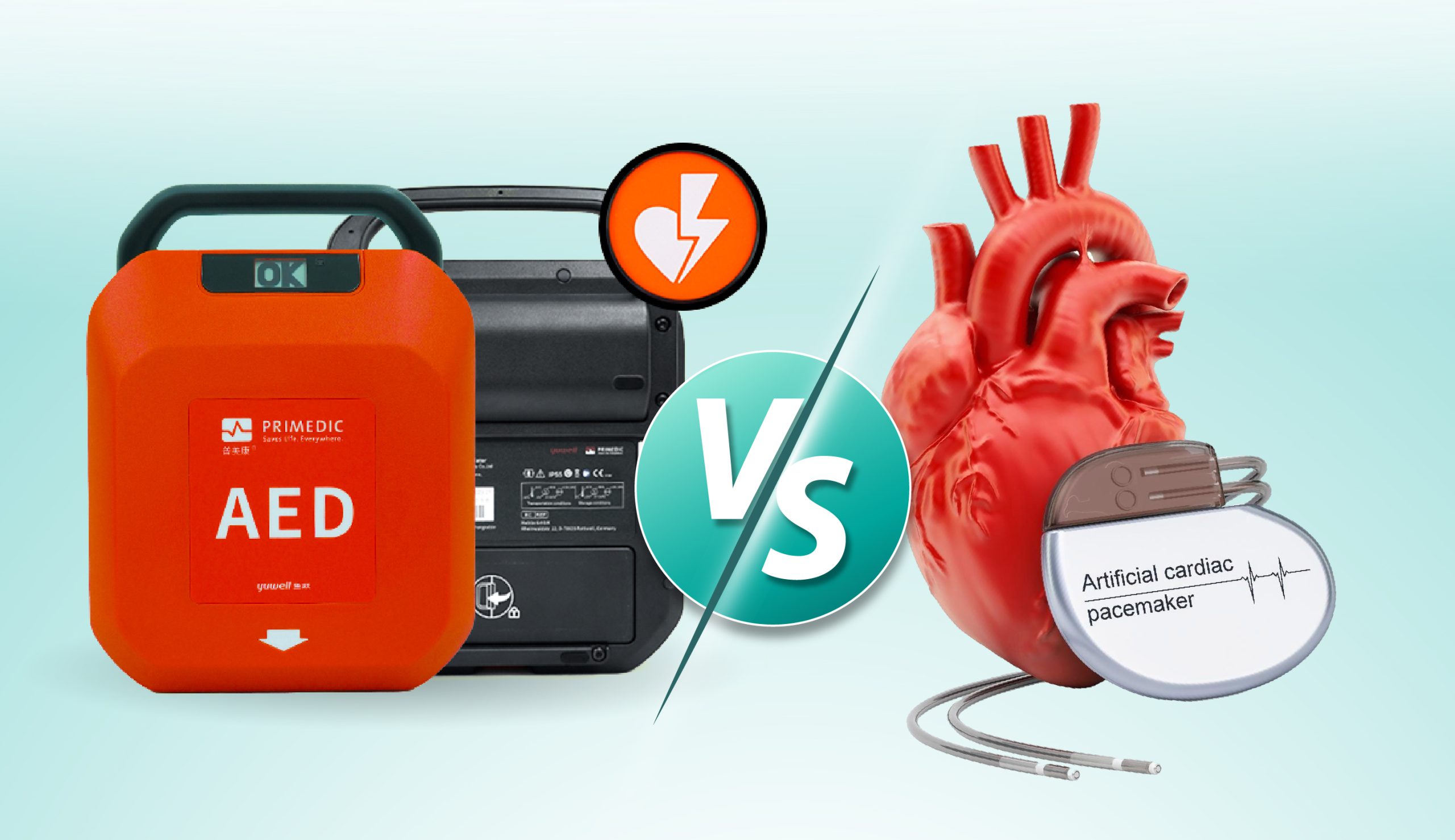
⚡ Pacemaker vs. AED: What’s the difference?
🔹 Pacemaker
-
How it works: Implanted permanently in the body, delivering small electrical impulses to keep a normal rhythm.
-
Best for:
-
Bradycardia (slow heart rate)
-
Chronic rhythm disorders
-
Heart failure with electrical dyssynchrony
-
-
Goal: Long-term rhythm control.
🔹 AED (Automated External Defibrillator)
-
How it works: External emergency device that analyzes rhythm and delivers a high-energy shock to reset lethal arrhythmias.
-
Best for:
-
Sudden cardiac arrest
-
Severe arrhythmias like ventricular fibrillation
-
-
Use cases:
-
Installed in public places—airports, schools, offices, malls.
-
Used together with CPR to save lives.
-
📊 Comparison table
| Feature | Pacemaker | AED |
|---|---|---|
| Usage | Implanted, long-term | External, emergency |
| Main role | Maintain steady rhythm | Shock for arrest/severe arrhythmia |
| Best for | Chronic heart conditions | Unresponsive, sudden arrest |
| Time frame | Long-term care | Acute only |
| Who applies | Implanted by physicians | Laypeople can use (voice prompts) |
🛒 Where to buy a pacemaker or AED?
-
Hospitals and leading clinics – Standardized care with physician guidance.
-
Medical equipment stores – Choose those with clear certifications.
-
Authorized distributors – Check CE, FDA, and local approvals.
-
Consult physicians or experts – To select the right type and model for your condition and budget.
💚 Why choose FASICARE?
FASICARE is a complete center for medical and elder/patient-care devices:
-
Products certified to international standards (ISO13485, IEC, CE)
-
Expert team support and after-sales service
-
Fast delivery with hands-on user training
-
Consultation on both products and practical health knowledge
✨ Your health and safety—and your family’s—come first. Fasicare is here by your side.
